Clinical Trials

A clinical trial is a research study conducted in human beings with the goal of answering specific questions about new therapies, vaccines or diagnostic procedures, or new ways of using known treatments. Clinical trials are used to determine whether new drugs, diagnostics or treatments are both safe and effective. Carefully conducted clinical trials are the fastest and safest way to find treatments that help people.
A clinical trial in the European Union is defined by Directive 2001/20/EC, as a clinical study that aims to investigate the therapeutic effect(s) of medicinal products that have not yet been authorized by regulatory bodies such as the European Medicines Agency (EMA), or the value of authorized drugs in cases other than those for which it has been authorized. In addition, clinical trials are considered those studies that seek to assign specific products to a therapeutic strategy or propose to investigate effective diagnostic or monitoring procedures.
What Are the Different Phases of a Clinical Trial?
A new therapy/drug cannot enter the market unless tested in the context of a clinical trial and found to be safe and effective. Clinical trials have three phases (I-III), preceded by a pre-clinical (laboratory phase) and often a post-marketing phase where data are still collected.
For every new drug/compound that finally enters the markets, thousands of different compounds have been designed and rejected in the pre-clinical phase. Moreover, only about 10% of drugs that enter clinical trials actually get authorised, as they have to prove safe, effective and better or equally good as current standard treatment.
Drug development procedure, including pre-clinical phase and clinical trial, normally takes about 10-15 years and takes place within a well-defined and heavily regulated framework.
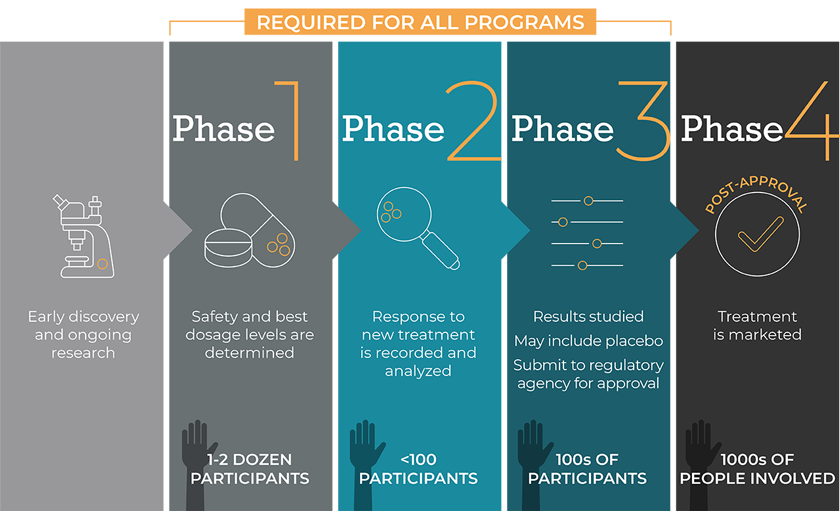
Phase I: Screening for safety. Testing within a small group of often-healthy people (typically 20–80) to evaluate safety, determine safe dosage ranges, and identify side effects.
Phase II: Establishing the preliminary efficacy of the drug in a “treatment group”, usually against a placebo control group. It includes more people (100 to 300). While the emphasis in Phase I is on safety, the emphasis in Phase II is on effectiveness. This phase aims to obtain preliminary data on whether the drug works in people who have a certain disease or condition. These trials also continue to study safety, including short-term side effects. Phase IIa is specifically designed to assess dosing requirements (how much drug should be given), while a Phase IIb trial is designed to determine efficacy, and studies how well the drug works at the prescribed dose(s), establishing a therapeutic dose range.
Phase III: Final confirmation of safety and efficacy. Testing with large groups of people (typically 1,000–3,000) to confirm its efficacy, evaluate its effectiveness, monitor side effects, compare it to commonly used treatments, and collect information that will allow it to be used safely. Upon successful completion of Phase III, an application is filed at the regulatory authorities (EMA in Europe, FDA in USA) for approval of the new drug.
Phase IV: Safety studies during sales. Post marketing studies delineate risks, benefits, and optimal use. As such, they are ongoing during the drug’s lifetime of active medical use.
An Authorised Medicine’s Journey:
The European Medicines Agency (EMA)’s booklet ”From laboratory to patient: the journey of a centrally authorised medicine” is useful and comprehensive resource that describes the journey of a medicine for human use authorised through EMA, from initial research to discussions on patient access to medicines across the EU.
In particular, this useful informative guide describes how EMA supports medicine development by providing scientific advice and how it assesses a medicine’s benefits and risks once it receives an application for marketing authorisation, including details on scientific advice, medicines’ evaluation and discussion at national level on access and pricing.
Read/Download the Booklet
Best Practices Guidance for Clinical Trials
 In September 2024, the World Health Organization (WHO) released groundbreaking guidelines to strengthen the design, conduct, and oversight of Clinical Trials globally.
In September 2024, the World Health Organization (WHO) released groundbreaking guidelines to strengthen the design, conduct, and oversight of Clinical Trials globally.
This initiative aims to bolster country-led research and development (R&D) ecosystems, making innovative, safe, and effective health interventions more accessible and affordable for everyone, faster than ever before.
The Guidance addresses key challenges such as poor trial design, limited participant diversity, inadequate infrastructure, and bureaucratic inefficiencies.
Read/Download the Guidance
Why Participate in a Clinical Trial?
There are many reasons why people choose to join a clinical trial. Some join a trial because the treatments they have tried for their health problem did not work. Others participate because there is no treatment for their health problem. By being part of a clinical trial, participants may find out about new treatments before they are widely available. Some studies are designed for, or include, people who are healthy but want to help find ways to prevent a disease, such as one that may be common in their family.
Many people say participating in a clinical trial is a way to play a more active role in their own health care. Other people say they want to help researchers learn more about certain health problems. Whatever the motivation, when you choose to participate in a clinical trial, you become a partner in scientific discovery. And, your contribution can help future generations lead healthier lives. Major medical breakthroughs could not happen without the generosity of clinical trial participants—young and old.
Also See:
All new therapies/drugs that enter clinical trials are listed in specialized portals, where one can find all relevant information.
https://clinicaltrials.gov/ https://www.clinicaltrialsregister.eu/
Up-to-date information on clinical trials for new therapies related to thalassaemia and sickle cell disease can be found HERE.